Understanding Sleep Apnea Syndrome: A Comprehensive Overview
Sleep Apnea Syndrome (SAS) stands as a formidable respiratory disorder, intricately woven into the fabric of our physiology. At its core, SAS primarily stems from the partial or complete obstruction of the upper airway. Yet, it can also arise when the brain fails to relay appropriate signals for respiratory function, leading to occurrences of hypoventilation or apnea. The complexity of SAS lies in its multifaceted pathophysiology, marking its significance in sleep medicine.
Pathophysiology of Sleep Apnea Syndrome
The mechanisms driving SAS are varied and interconnected. Key factors include anatomical abnormalities within the upper airway, neurological dysregulation, and muscular dysfunction. Each of these elements forms a crucial piece of the larger puzzle that contributes to the breathing difficulties experienced during sleep. In extreme cases, patients may present with a combination of these factors, further complicating the diagnosis and treatment.
Large-scale community studies have shed light on the prevalence of Obstructive Sleep Apnea (OSA), revealing startling statistics. Research indicates that 26% of adults encounter some form of sleep-disordered breathing, with prominent risk factors including age, gender, body mass index (BMI), hypertension, and smoking history.
The Nightly Experience of SAS Patients
During the night, individuals suffering from SAS often experience reduced airflow alongside significant declines in blood oxygen levels. These nocturnal episodes of apnea can occur repeatedly, leading to fragmented sleep and frequent awakenings. Consequently, patients find their nighttime rest severely compromised, which, in turn, impacts their overall daily functioning.
Chronic disruptions from sleep fragmentation and hypoxemia aren’t merely inconvenient; they usher in a range of physiological and psychological issues. Cognitive dysfunction, mood swings, and an overall decline in quality of life are commonly reported among those with SAS. The consequences extend beyond simple fatigue; chronic sleep disturbances tie closely to various health outcomes, including cardiovascular disease, where SAS is now recognized as a significant risk factor.
Cardiovascular Implications of SAS
SAS is intricately linked to a variety of cardiovascular conditions such as hypertension, arrhythmias, coronary artery disease, and stroke. The repeated bouts of hypoxia and sleep fragmentation initiate systemic inflammatory responses and oxidative stress, leading to potential cardiovascular dysfunction. The impact of SAS is compounded by the association with metabolic disorders, further underscoring its critical relevance in modern health discussions.
Research has tied SAS to insulin resistance and type 2 diabetes, amplifying the health burden on affected patients. The relationship between sleep quality and metabolic health is an area ripe for exploration, as the implications stretch across demographics, affecting millions worldwide.
Diagnosis: The Role of Polysomnography
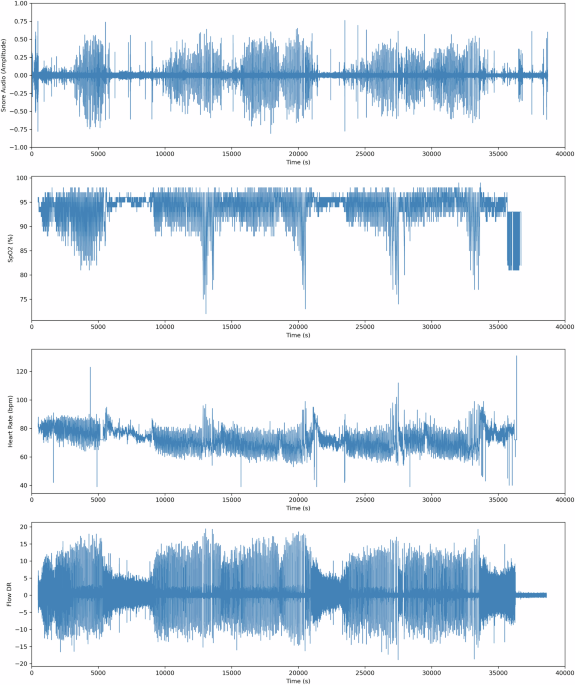
Currently, polysomnography (PSG) stands as the gold standard in diagnosing OSA. This comprehensive monitoring process tracks a host of physiological parameters, including airflow, blood oxygen saturation, respiratory effort, and brain activity. By analyzing these factors, clinicians can assess the severity of OSA with considerable accuracy.
However, the logistics surrounding PSG pose significant challenges. Conducted primarily in controlled sleep laboratories, patients often face discomfort from wearing multiple sensors. Unfamiliar environments can lead to artificially altered sleep patterns, resulting in data that doesn’t accurately represent true sleep health. Consequently, patient compliance can plummet, highlighting an urgent need for more accessible diagnostic strategies.
The Future of Diagnostics: Portable Monitoring Solutions
To address these pressing challenges, innovative approaches are emerging. Using portable devices, such as smartphones, in conjunction with advanced deep learning algorithms is becoming a viable solution for continuous monitoring of sleep health. This development aims to provide a non-invasive method for disease detection while enhancing patient compliance and convenience.
Public datasets have been foundational in shaping research methodology, yet many rely on high-quality audio and multimodal data derived from PSG. These datasets often don’t reflect the realities of home environments, leading to significant hurdles in practical applications. Notably, audio collected through portable devices often comes with limitations in quality, underscoring the need for adaptations in deep learning models for effective deployment.
Building Robust Datasets: A Step Forward
Recognizing the demand for improved data fidelity, efforts are underway to construct high-quality sleep datasets that closely resemble real-world conditions. This initiative aims to support the development of deep learning-based algorithms tailored for smartphone audio applications. Researchers have embarked on significant data collection endeavors, capturing audio from patients using smartphone microphones in natural settings. Coupling this with PSG information allows for detailed annotation of snore-related events, while also retaining vital physiological metrics.
This new dataset, encompassing over 400 hours of sleep audio collected from 50 patients, aims to bridge the existing gap between PSG data and smartphone recordings. By enhancing data quality and availability, researchers hope to propel the development of robust, portable OSA monitoring algorithms, thereby improving patient management and treatment options.
Impacts of Continuous Monitoring on Patient Care
With ongoing advancements in smart technology, the horizon of sleep apnea diagnosis and management is widening. Portable monitoring systems offer patients the opportunity for continuous, real-time tracking of their health, leading to a more personalized approach to care. Such innovations promise to not only enhance diagnostic accuracy but also offer an avenue for patient self-management, potentially transforming the landscape of sleep medicine.
In this evolving field, the intersection of technology and health management continues to hold promise for those suffering from Sleep Apnea Syndrome, paving the way for a future where sleep health can be monitored effectively and conveniently from the comfort of one’s home.